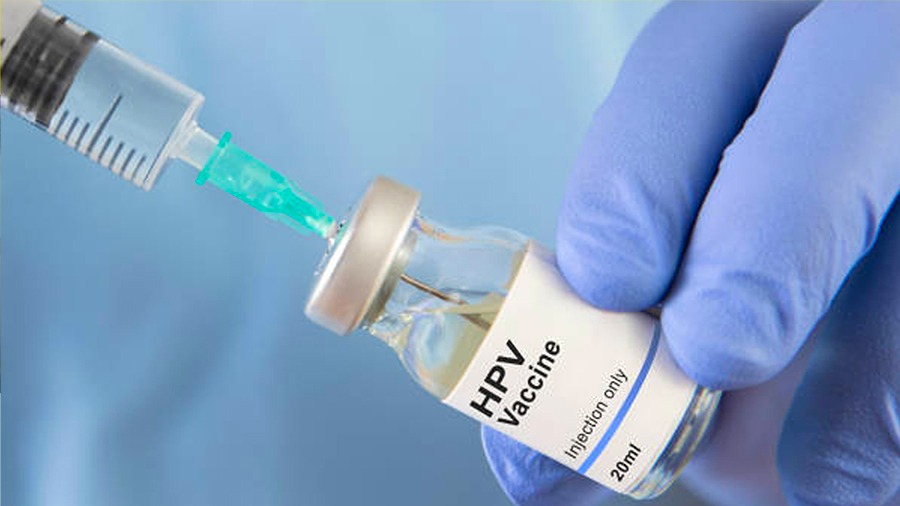
Why do we need HPV Vaccines?
The Human papillomavirus (HPV) is a common sexually transmitted infection that can lead to serious health issues, including cervical cancer and genital warts. The HPV vaccine has been proven to prevent and protect against several high‐risk HPV strains which cause these conditions. Early vaccination is necessary for boys and girls aged 9 to 26. Vaccination at these ages is crucial for maximizing immune response and preventing HPV‐related diseases. While the vaccine is effective up to age 45, early immunization provides the best protection.
What is HPV?
HPV is a widespread virus with over 100 strains, some of which are linked to cancer and genital warts. It is mainly spread through sexual contact and is very common among sexually active individuals. HPV types 16 and 18 are responsible for about 70% of cervical cancer cases worldwide. The strains 6 and 11 cause genital warts. In people with a good immune system, the virus can clear spontaneously in about 2 years. But persistent infections can lead to precancerous lesions and cancer.
What are the 5 reasons to get HPV vaccines?
Reason 1: Prevent Cervical and Other Cancers .
The HPV vaccine is primarily aimed at preventing cervical cancer. It can also prevent other cancers such as anal, mouth and throat cancers. Studies have shown that vaccination significantly reduces the risk of these cancers by targeting high‐risk HPV types like 16 and 18. For example, Gardasil 4 protects against the 4 main strains of HPV – 6,11, 16 and 18. Gardasil 9 protects against 9 strains. Regular screening remains important even after vaccination, since cancers can sometimes (rarely) be caused by other HPV strains not prevented by the HPV vaccine.
Reason 2: Prevent Genital Warts
The HPV vaccine also protects against strains 6 and 11, which are responsible for most cases of genital warts. While Genital warts are not dangerous per se, they can cause significant physical discomfort and emotional distress. The HPV vaccine is quite effective in preventing these warts. This improves both physical and mental health. It has been seen that vaccinated people rarely have genital Warts.
Reason 3: Early Vaccination Maximizes Immune Response
Vaccination at a young age, typically between 9 and 26, maximizes the immune response to HPV. This pre‐exposure vaccination ensures that individuals are protected before they become sexually active, reducing the risk of infection. While the vaccine can still be effective if administered later, up to age 45, early vaccination provides the best protection.
Reason 4: Proven Vaccine Safety and Efficacy
The HPV vaccine has proven to be very effective as well as safe. Common side effects are mild and temporary, such as pain at the injection site or slight fever. Major health organizations, including the WHO and CDC, endorse the vaccine based on its favorable safety profile. No evidence has been found linking the HPV vaccine to serious long‐term side effects.
Reason 5: Improves Herd Immunity.
HPV vaccination not only protects the individual but also contributes to herd immunity – this reduces the spread of HPV in the community. This collective protection benefits both vaccinated and unvaccinated individuals, particularly those who cannot receive the vaccine due to health reasons. Encouraging others to get vaccinated helps maintain public health and prevents HPV‐related diseases.
Frequently Asked Questions (FAQs)
How does the HPV Vaccine Work?
The HPV vaccine works by using virus-like particles (VLPs) that mimic the outer shell of the HPV virus but lack its genetic material. Since they do not have the genetic material, the vaccines cannot cause an infection. VLPs stimulate the body’s immune system to produce antibodies that can recognize and neutralize the actual HPV virus, providing protection against infections caused by the different strains. This mechanism is highly effective in preventing persistent infections that can lead to cancer and other diseases.
What are some common HPV Vaccine Myths?
Several myths surround the HPV vaccine, but scientific evidence has proved them to be false:
Myth 1: HPV vaccination is unsafe.
Fact: The vaccine is extensively tested and monitored, with side effects typically being mild and temporary.
Myth 2: HPV vaccination causes infertility.
Fact: There is no evidence linking the HPV vaccine to infertility; it can actually protect fertility by preventing cervical cancer treatments
Myth 3: It is not necessary if you get regular pap smears
Fact: Pap smears daignoze changes in the cervical cells. They cannot prevent HPV infections. HPV vaccines are necessary to prevent the infection.
Myth 4: The HPV vaccine is only for women
Fact: The HPV vaccine is necessary in both men and women. In men, they help prevent genital warts as as well as prevent cancers of the mouth or anus caused by the HPV virus.
Myth 5: The HPV vaccine is only effective in people who have never been sexually active.
Fact: The vaccine is most effective when given to children and adolescents before they are exposed to the virus, but it can still benefit adults up to age 45.
Myth 6: A women who has received the HPV vaccine does not need pap smears
Fact: HPV vaccines does not remove the need for pap smears since the cervical cancers can be caused by other HPV strains or by other factors.
Myth 7: You can’t receive the HPV vaccine if you’ve already been infected
Fact: There are more than 100 types of HPV; the vaccine covers nine of the most prominent strains, which are linked to nearly 90% of cancers and genital warts. You may be infected by one strain but you need to be protected against the others.
Myth 8: You do not need to use birth control methods like condoms to protect against HPV if you get the HPV vaccine.
Fact: It is always better to use condoms for a second layer of protection against HPV.
HPV is one of the most common sexually transmitted infection and it is important that all vulnerable people are vaccinated against it.